HRS describes a narrowing of the lumen of the urethra. It has various causes and is mainly caused iatrogenically, as a result of urethral manipulation.1 Men are predominantly affected by this condition. After the age of 55, the incidence of this condition increases sharply.2,3 Various surgical procedures are available to treat the stenosis.
These include dilatation of the stenosis (bougienage), endoscopic slits (urethrotomia interna), and various open-surgical urethroplasty techniques.4
Table 1: Overview of different methods for the treatment of urethral stricture (Tritschler et. al)5
|
Endoscopic therapies |
Open surgical procedures |
|
|
In the following chapters, the current minimally invasive standard procedures, bougienage and slitting, as well as the open surgical procedures are presented, their advantages and disadvantages are highlighted, and the efficiency of the therapy alternatives is discussed. In addition, a comparison of these methods with treatment using the biotechnologically produced tissue substitute MukoCell® is provided.
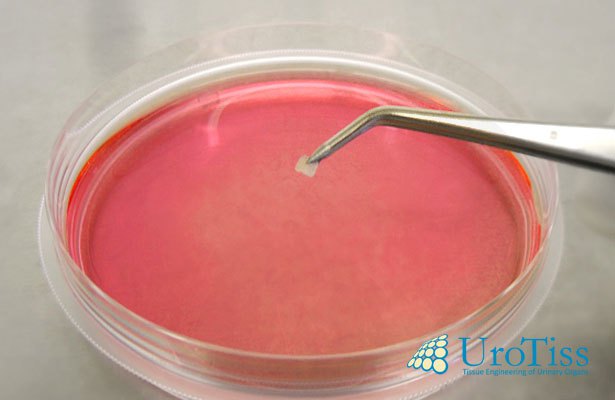
Urethral reconstruction with the autologous patient-derived cell graft MukoCell® is a gentle alternative to conventional transplantation with native oral mucosa. The tissue substitute, grown from the patient’s own cells, integrates into the surrounding tissue within a short time and develops into new, fully functional urethral tissue. To obtain the graft, a small piece of the oral mucosa is removed from the patient under local anesthesia (see figure).
Small biopsy instead of large-scale removal of oral mucosa.
For patients, the use of the autologous graft has decisive advantages, as the biopsy is largely painless and free of complications. The conventional large-area removal of native oral mucosa and the associated complications (pain, bleeding, discomfort, contractures, deformation of the mouth, difficulties in eating, drinking and speaking, permanent salivation, …) are eliminated. Moreover, the removal of only a few cells from the oral mucosa shortens the operation and anesthesia time, thus simplifying the surgical technique. The costs for the use of the transplant and the care of the patient remain the same.
Urethral reconstruction with native oral mucosa is a method of treating urethral strictures. However, the usually extensive removal of oral mucosa from the patient’s cheek carries associated complications such as pain, bleeding or scarring with possible consequences for facial expression, food intake, mobility of the lower lip. Current statistics indicate complications from oral mucosa harvesting in 18%-30% of patients. Also, harvesting native oral mucosa from the patient’s cheek is limited.
Due to the oral complications and the lack of evidence-based data to date, urethral reconstruction with native oral mucosa is not a good method for the treatment of urethral strictures.
Slitting is the most commonly used method for urethral stenosis. In Germany alone, approximately 45,000 procedures are performed each year, with many patients receiving multiple treatments. The procedure is quick to perform and is less expensive per procedure relative to other treatment methods. However, the 12-month failure rate in this case is 70%, and in the case of repeated slits, the chances of recovery even drop to as low as 0%: After each treatment repetition, the probability of a re-stricture increases [Steenkamp et al 1997, Santucci 2009]. Thus, a patient has to be treated several times over his lifetime (sometimes 2-3 times per year).
For this reason, urethrotomy/slitting, which can only be used temporarily, is not considered a useful method for treating urethral strictures.
| 1 | Lumen et al. Etiology of urethral stricture disease in the 21st century. The Journal of urology, 182:983-987. |
| 2 | McMillan A, Pakianathan M, Mao JH, Macintyre CCA. Urethral stricture and urethritis in men in Scotland, Genitorium Medicine. 1994; 70(6):403–405. |
| 3 | Santucci and Eisenberg. Urethrotomy has a much lower success rate than previously reported. The Journal of urology. 2010; 185(5):1859-1862. |
| 4 | Rohwer AE. Langzeitergebnisse und Lebensqualität nach Rekonstruktion der Harnröhre mit Mundschleimhaut, Dissertation, Medizinische Fakultät der Universität Hamburg, 2015. |
| 5 | Tritschler et al. Harnröhrenstrikturen – Ursachen, Diagnose und Therapien. Deutsche Ärzteblatt International. 2013; 110(13):220-226. |